
UNDERSTANDING OUR “WEAR ZONES”

Vincent Hanneken, PT/Owner
By Vincent Hanneken, PT/Owner
Hello and welcome to our osteoarthritis (OA) or another way to say it is Degenerative Joint Disease issue of our newsletter. This is a condition nearly everyone to some degree is going to experience. The question is how will they address it? The data below provides some understanding of where we are now as a country regarding the use of surgery to address the end stage of arthritis. And, we have several articles to help you understand how graded exercise helps to stimulate the mechanism whereby cartilage can recover better from the stress of activity.
In the US, 1.3 million total knee replacements (TKA) in 2023 were performed; it is the most common orthopedic surgery and comprises 40% of the total number done per year worldwide which is interesting since the US only makes up 4.3% of the world population.
When comparing the USA to Canada, countries that have similar demographic and economic situations, the US does about 50% more TKAs than Canada per 100,000. And not so unsurprising, the projection is for this number to significantly grow by 2040 for TKAs in the US. Total hip replacement (THA) in 2023 amounted to over 760,000, and lower back surgeries for laminectomies and/or fusion numbered 500,000. Shoulder surgeries for rotator cuff repair was nearly 500,000 and cervical surgeries for relieving nerve compression was around 135,000/yr.
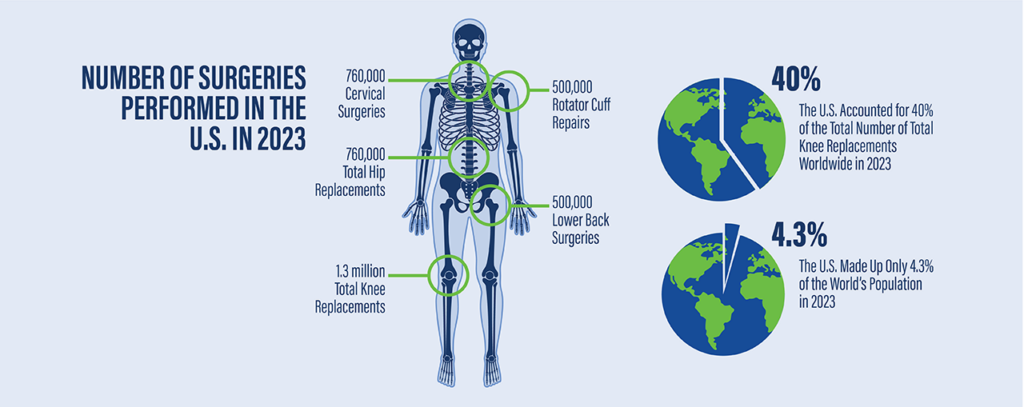
It is amazing we have the technology to help people whose joints are so degenerated a replacement is needed to sustain their quality of life; however, the projected number of these surgeries is going to grow at an even faster rate than the past 25 years. Between 2000 and 2019, the estimated annual volume of THAs increased by 177% and that of TKA increased by 156% on average. Based on this data, it’s not hard to draw a conclusion that the US has a major problem with arthritis and how it is handling this disorder.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9974080
It is clear based on these stats that the human body has common “wear zones” and we can see from the frequency and type of surgeries what areas of the body are vulnerable to degenerative joint changes.
Cartilage is the tissue that overlies our joint surface and is vulnerable to wearing down and creating a bone-to-bone condition which is called degenerative joint disease or OA. Knees are number one for surgery, followed by hips, lower back, shoulders and then the cervical spine and from treating many patients in therapy this pattern seems accurate.
This data on surgeries and joint replacements indicates quite clearly where our vulnerable areas are in our body.
The question becomes what could we do to reduce the stress in these “wear zones” and help lower our chances of becoming an eventual candidate for surgery to replace a worn-out joint.
The optimal condition is for our joints to age at the same rate or even slower than our chronological age; yes, I am 65 but the doctor says my joints on x-ray looks like I am 50. Wow, how could we improve our odds to hearing that from our physician? In our country, the opposite condition is occurring more and more as the statistics mentioned earlier indicate. A common denominator to many arthritic joints is that restrictions and poor muscle control over the joint are insidiously occurring over time to wear the cartilage faster than it can repair itself.
It may not be recognized by someone, but our bodies are in a perpetual dynamic between forces that are causing the body to breakdown and our immune system’s potential to repair and manage this breakdown to sustain health. These wear zones are places where the repair cycle is not keeping up with the breakdown due to the concentration of stress.
From a physical therapist point of view, if those wear zones were managed early in the stress cycle and the patient is educated on how to care for their unique vulnerable areas, their ability to keep their rate of healing ahead of breakdown would be improved.
A PT’s exam can help identify why stress is concentrating over a joint causing pain and inflammation.
Their exam can look at the system of movement, called the kinetic chain, to see where the weak and tight links are which are causing stress on a knee, hip or lower back.
A PT is really the only professional who assesses a patient as a system of movement which is how the body functions. In so doing, they can get an understanding how to treat the involved area and reduce stress to the joint that is not keeping up with the repair cycle. It is a strong fact that the earlier in the degenerative process you take action to treat an area to alter the rate of breakdown back to favor the repair cycle, the easier and more successful the process is.
The rest of this issue is devoted to helping you understand the role of cartilage in your joints and how correct exercise can improve the ability of our cartilage to take stress and not suffer.
It is sometimes surprising to a patient to come to understand that exercise can be therapeutic and healing to a joint when it seemed that activity caused it to get sore in the first place. Over utilizing rest is not the answer or nor is the excessive use of anti-inflammatory drugs. Neither assist with improving the integrity of the cartilage.
I would encourage you to read on to get a better understanding of how graded pressure with prescribed exercises can help a joint recover to perform better during your day. With being more proactive before the joint is fully worn out, one can improve their chances that a total joint replacement is not waiting for them as they move into their 6th decade or later.
To healthy joints,
Vincent Hanneken, PT

Promote Cartilage Health (Sponge Analogy)
By Dr. Luke VanderZouwen, Doctor of Physical Therapy

Doctor of Physical Therapy
Cartilage is a substance that lines our joints and it provides cushioning, lubrication, and a smooth surface so that your joint can move in a relatively effortless fashion. It is typically made up of 60-80% water. The other 20-40% of cartilage is a mix of different protein structures, with the most commonly known being collagen. Like most other tissues in our body, cartilage requires nutrients to stay healthy. Tissues, like muscle, skin, or bones, get most of these nutrients through blood flow. Cartilage is a bit different. It gets nutrients from turnover of joint fluid. To help better understand this process, I like to think of cartilage like a sponge that lines our joints (Hear me out…I’ll explain more in the next 2 paragraphs).
Imagine a counter that just had a glass of water spilled on it. Now take a dry dish sponge and place it in the middle of the water spill. If I just let it sit, a little bit of the water will soak into the bottom of the sponge, but the top of the sponge will probably stay dry. Next take your hand and compress the sponge against the counter. Do this 4-5 times and what happens? The sponge soaks up some of the surrounding water and no longer feels dry. In this example, the sponge is like your cartilage and the water is like joint fluid. As the sponge (cartilage) is compressed, the water (joint fluid) is pushed out of the sponge and then soaked back in when the sponge (cartilage) is released. This pumping phenomenon is very similar to how joints work when they are compressed, usually through weight bearing activity/exercise. The pump action will squeeze out waste products and then soak up nutrients from our joint fluid. In this way, the cartilage in our joints can either stay healthy or miraculously can even heal itself.
Now let’s say you have an old, well-used, dried-out dish sponge. It might have some little cracks, a couple of holes, and is probably thinner than an otherwise new sponge. If I were to take this dry sponge and run my fingernail over it, it might even catch some of the little cracks and make a scratchy kind of noise. If I take this sponge and place it on the counter and work the pumping action, that same sponge will no longer feel as dry or scratchy and I might not even catch my fingernail anymore. It might even plump up a bit and not look as thin. This sponge is an example of cartilage within a joint with some osteoarthritic changes. It gets its nutrients from exactly the same process as healthy cartilage (a new sponge). More and more research is building to show that cartilage, even cartilage that is thin or has small holes or cracks, has the ability to heal.

Weight bearing is very important for promoting health in cartilage, but as with most things in life, moderation is key. If a joint is painful with weight bearing, there could be many reasons why. Movement mechanics, inflammation, cartilage health, strength in surrounding muscles, tendon health, and sensitivity in any of the structures around the knee can play a role in difficulty with bearing weight. A gradual build up process to weight bearing activity or compressive exercise is important to build capacity in the structures surrounding a joint and to reduce sensitivity if painful.
If the sponge analogy makes sense and you are looking to promote long term health in your cartilage, but you are having a difficult time knowing how to begin or if pain is limiting your abilities, a physical therapist may be able to help. Physical therapists are highly trained in pain management related to movement and are experts in prescribing individualized exercise regimens to promote health, including health in cartilage. It is time to take care of those “sponges!” A physical therapist may be able to help. At Full Potential, we provide free consultations to discuss just these types of situations!
Call us at 616-537-2864!
DO YOU NEED A TUNE UP?

Getting back into action after a long winter full of snow like this one may be a challenge. It is amazing how much we can lose from a few months of being more sedentary! Even though snow is still on the ground, spring is not far off and nature will be calling you out to play and work. What could you do now? Well, consider a tune up at Full Potential. By addressing a problem in its infancy a quicker recovery can occur and you will not risk wasting valuable warm weather time by putting excessive stress on unprepared joints and muscles, potentially causing a strain on that first warm day. This is certainly not the way to start the warm weather season.
We are here to help you have a smooth transition back to an active lifestyle. Not sure if you need help? That’s easy – come in for a FREE CONSULTATION and we can talk, test to identify deficits and discuss what may be needed. We also offer consultations by phone, just call 616-537-2864.

Spotlight on Research:
Exercise Can Help with Osteoarthritis and Comes with Added Bonuses!
Exercise and physical activity can be difficult to navigate in light of arthritic changes in one’s body, especially when those arthritic changes may be associated with painful joints. A clinical commentary titled Physical Activity and Exercise Therapy Benefit More than Just Symptoms and Impairments in People With Hip and Knee Osteoarthritis, attempts to clarify the effect the right type of exercise can have on not only symptoms of osteoarthritis, but also a number of other health issues.
Over and over again exercise is seen to improve symptoms of osteoarthritis, including pain, stiffness, and poor physical function. The beauty of exercise is that it has very few potential negative side effects. When compared with analgesics (pain medication like Tylenol, ibuprofen, narcotics, etc), injections, and surgeries, the risks associated with exercise are minimal. Sometimes if dosed inappropriately, exercise can cause more in the moment soreness, but is rarely associated with injury. Exercise has also been shown to consistently reduce the risk of developing 35 chronic conditions and can help with treatment of at least 26 of these conditions. Some of these health issues include cardiovascular disease, type II diabetes, and various mental health related diseases. Exercise therapy is low risk and has high potential reward!
There are certain consistencies in exercise therapy that should be considered when starting up a routine for individuals with hip and/or knee osteoarthritis. Some of these features, as outlined by this clinical commentary, can be seen in the table below.* These 7 recommendations can be self-guided, but the research points to these recommendations being most effective when determined by a professional.
Physical therapists are well versed in these 7 recommendations and can provide individualized programs to work toward meeting your goals. If you are dealing with osteoarthritis and struggling to keep up a consistent movement routine as a result, I strongly encourage you to seek out help. Not only does this have the potential to improve your joint health and function, but also to improve your overall health and well-being. Scheduling a consultation with a physical therapist could be a great first step toward better health!
Seven Exercise Therapy Recommendations for Hip and Knee Osteoarthritis
Description
- Provide aerobic, resistance, performance, or neuromuscular exercises tailored and targeted to individual patient needs and preferences.
- Consider aquatic exercises in patients who are unable to adequately complete land-based exercises due to pain.
- Provide a minimum of 12 supervised exercise sessions of 30 to 60 minutes per session over a 6-week period (ie. 2 sessions per week).
- Encourage an additional 1 to 2 sessions per week to optimize outcomes, particularly related to strength.
- Consider extending initial exercise therapy programs to 12 weeks or longer to optimize outcomes, particularly related to strength.
- Include patient education and consider booster sessions in the long term to enhance adherence and progression.
- Provide education and reassurance about managing potential pain flares and inflammation, and how to modify exercises and physical activity to ensure continued participation.
*Skou ST, Pedersen BK, Abbott JH, Patterson B, Barton C. Physical Activity and Exercise Therapy Benefit More Than Just Symptoms and Impairments in People With Hip and Knee Osteoarthritis. J Orthop Sports Phys Ther. 2018 Jun;48(6):439-447. doi: 10.2519/jospt.2018.7877. Epub 2018 Apr 18. PMID: 29669488.



Full Potential Reached!
When a business consistently earns glowing reviews, it’s a testament not just to good service, but to exceptional quality as well. We thought we’d take a moment to highlight some of the enthusiastic 5 star reviews we’ve received recently that highlight what makes Full Potential stand out. Read on to see what Holland has to say about our clinic!
“As a result of coming to Full Potential, I am able to do activities without pain that caused me pain before – walk, run, stairs, and lifting. The clinic is personable, had a personal and practical approach with the things I can do that help/heal, and targeted my specific symptoms. I saw 100% improvement in my condition.”
—Thomas T.


“After PT, I no longer have pain stepping up, squatting, or bending. I no longer have pain when I sleep. I am not afraid of physical activity hurting my hips. I can ride my bike, walk, and play pickleball without pain. I improved 100%!”
—Jan M.
Inspiring Outcomes: More Patients Share Their Transformations
“No one WANTS to need physical therapy but when life decides otherwise I’d highly recommend the fine folks at Full Potential! I’ve been working with them for 2 months now… coming back from knee surgery… and I’ve found them to be professional, knowledgeable, supportive, and open. They are quick to answer questions, tolerate my curiosity about the “Why?” of certain treatments and exercises and in general have made this process as pleasant as possible. Highly recommended!”
“Efficient, professional, so knowledgeable and helpful. As a personal trainer and health coach I would recommend this place to everyone (and have!)”
“My experience at Full Potential PT has been far better than I had expected. Both therapists I worked with had creative ideas for approaching the problem from a different angle if one approach didn’t work. At each appointment I felt they listened to me intently and worked hard to make sure I understood the concepts behind their treatment. They paid attention to me as a person, as well as a client.”
“Very focused therapist, prompt and communicative. And the actual therapist was with me every minute – no assistants or techs. Been there for two rounds of therapy and would go back in a heartbeat.”
If you have had a great experience with us, we’d love to hear your feedback! Sharing your thoughts not only helps us grow and continue to provide excellent services, but it also helps others discover what makes Full Potential exceptional. Leave a review today and share your experience!
One Last Thought
A few weeks ago, I was cutting some trees and lifting logs and I knew I was going to be sore. Before bed I took some extra time and did some stretches for my hips, lower back and used a massage tool to my LB too. I could have taken some Ibuprofen and went to sleep but I chose to address more directly my pain with stretching and massage to improve how I would feel the next day. Surprisingly, I recovered faster than expected.
Knowing how to stretch and use techniques to loosen our joints improves circulation and it is the delivery of better blood flow that helps start the recovery process, then the restoration that occurs with sleep is more effective. Going to bed tight, just sets one up for stiffness and pain the following day as blood flow is not as free to deliver what our most tight areas need – oxygen and our immune system doing its job well as we sleep.
One needs to know how to stretch to address our vulnerable areas and have these techniques available in our tool box for days when we do too much as opposed to just using meds. This is another reason why PT is an investment that pays one back over time as you learn what to do for yourself in the future, when you decide to tackle a big job.
One can feed a man for a day or teach him to fish and feed him for a lifetime. Full Potential “teaches you how to fish.”
Best,
Vince Hanneken, PT
“A man too busy to take care of his health is like a mechanic too busy to take care of his tools.”
— Spanish Proverb

Feel Better by Eating Better!
Sheet-Pan Chipotle-Lime Shrimp Bake
Looking for a flavorful, no-fuss dinner packed with zesty spice and wholesome ingredients? This Sheet-Pan Chipotle-Lime Shrimp Bake is the perfect weeknight meal! Roasted baby red potatoes create a hearty base, while asparagus, Broccolini, and succulent shrimp are infused with a smoky chipotle-lime butter for a deliciously bold kick.
Ingredients
- 1-1/2 pounds baby red potatoes, cut into 3/4-inch cubes
- 1 tablespoon extra virgin olive oil
- 3/4 teaspoon sea salt, divided
- 3 medium limes
- 1/4 cup unsalted butter, melted
- 1 teaspoon ground chipotle pepper
- 1/2 pound fresh asparagus, trimmed
- 1/2 pound Broccolini or broccoli, cut into small florets
- 1 pound uncooked shrimp (16-20 per pound), peeled and deveined
- 2 tablespoons minced fresh cilantro
Preheat oven to 400°. Place potatoes in a greased 15x10x1-in. baking pan; drizzle with olive oil. Sprinkle with 1/4 teaspoon sea salt; stir to combine. Bake for 30 minutes. Meanwhile, squeeze 1/3 cup juice from limes, reserving fruit. Combine the lime juice, melted butter, chipotle and remaining 1/2 teaspoon sea salt.
Remove pan from the oven; stir potatoes. Arrange asparagus, Broccolini, shrimp and reserved limes on top of potatoes. Pour lime juice mixture over vegetables and shrimp.
Bake until shrimp turn pink and vegetables are tender, about 10 minutes longer. Sprinkle with minced fresh cilantro.
www.tasteofhome.com/recipes/sheet-pan-chipotle-lime-shrimp-bake/
Exercise of the Month
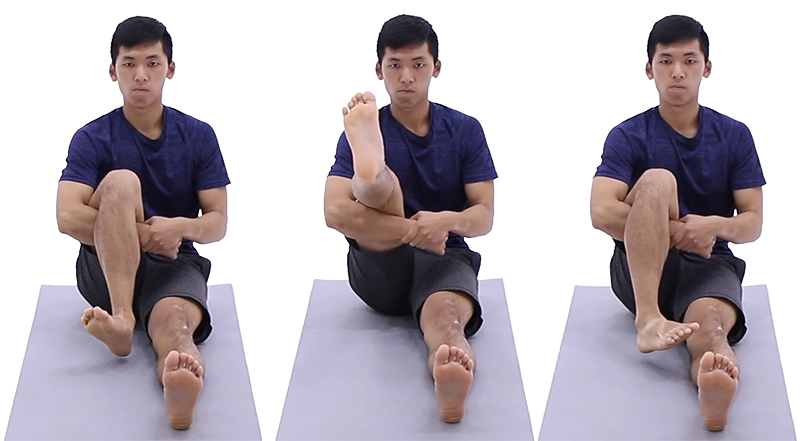
Knee Controlled Articular Rotations
Start by sitting on the ground with one leg straight and your other leg raised slightly resting on your forearm. Your heel should not be touching the floor. Turn your foot out as far as possible at your ankle and then extend your knee as much as possible. Turn your foot inward as far as possible and bend your knee as much as possible.

Let’s Get You Better ASAP!
Don’t let pain dictate your life. Take the first step towards reclaiming your mobility and well-being with our expert support. Start your journey to a healthier you today.






