
Why Your Knees Need a Good PT

Vincent Hanneken, PT/Owner
By Vincent Hanneken, PT/Owner
We treat many postsurgical patients, and one of the most common procedures we help people with is a TKA (total knee arthroplasty), where someone essentially receives a new knee. Everyone is different, but on average it’s a 4–8-week process to return to a functional level where they can self-manage. The initial goal for someone with this procedure is restoring their range of motion, as this is the foundation for rebuilding strength and function to return to usual activities.
It may be surprising to learn that in the U.S., about 1.3 million TKAs were done in 2023, at a cost of about $39 billion. Of all TKAs done worldwide, the U.S. accounts for 40%, despite being only 4% of the global population. Interesting, isn’t it, how much more per capita this procedure is done here than elsewhere? For example, compared to Germany—a similarly developed country—we did 2.4 times more knee replacements per capita in 2023.
What Can We Do to Slow This Trend?
One might ask: what can we do to slow down the rate of needing this surgery once we reach our 50s and 60s? Projections show that by 2040, TKAs in the U.S. could exceed 3 million annually—a 230% increase over current levels, which are already 2.4 times higher per capita than Germany. This raises valid questions: Will Medicare and insurance be able to support the cost increase? Will there be enough surgeons? How long will the wait be as demand rises?
Considering the rising costs of managing chronic diseases and the current $2 trillion U.S. annual deficit (to put it in perspective, one trillion is a million millions!), we must ask how long this can be sustained. As a result, this article is really aimed at those in their 40s, who may be TKA candidates in the next 15 years. Of course, technology may change the outlook. New procedures could reduce the need for or the cost of TKAs, but the old saying still applies: “An ounce of prevention is worth a pound of cure.”
Reducing Your Risk
It takes initiative to think preventatively, but it’s worth asking: what can you do now to reduce stress on your knees? Ideally, your joints should age more slowly than your chronological age. If you’re 60 and your knees function like a 45-year-old’s, that’s excellent. Sadly, we often hear the reverse, especially about our loadbearing joints: “You have the spine of an 80-year-old, and you’re only 50.” Sobering news.
Keep in mind, a knee replacement is not a pleasant procedure! In terms of pain and limitations, it’s often worse than a total hip replacement in getting back to reasonable function.
Joints are classified into categories. The knee is a hinge joint, meaning it moves mainly in one plane. Our fingers and ankles are other examples. More specifically, the knee is a modified hinge joint, with a small degree of rotation—but generally, rotation is not the knee’s friend.
Two Types of Knee Stress
- Traumatic – due to a specific event, like an accident or a fall
- Degenerative – a breakdown over time from work, sports, and everyday use
We’re focusing on the latter, but that’s not to say people with previous injuries shouldn’t also think preventatively. They should even more so, especially if they’ve already had surgeries, which are common precursors to eventual TKA.
Home Screening Tests
When thinking of prevention, there are two key areas to be attentive to when it comes to the knee’s range of motion: extension (straightening) and flexion (bending). Try these home screening tests to see how your range of motion is looking.

Flexion Test:
Lie on your back on a flat surface. Bending your knee, pull your heel towards your hip. Measure the distance between your heel and your hip. Repeat on the other side and compare. Normal flexion is about 140 degrees, or about 3–5 inches between hip and heel. How do your knees measure up?
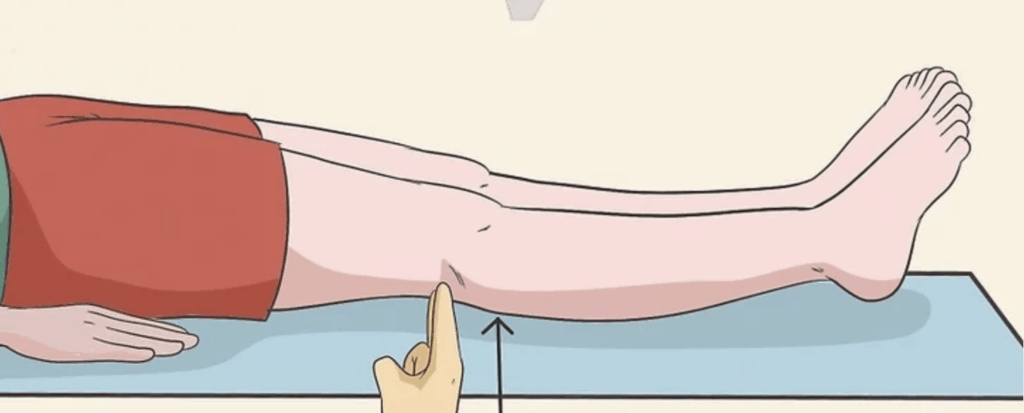
Extension Test:
Laying on a flat surface, extend your legs straight. Measure the distance between the underside of each knee and the floor. Ideally, there is no space between the two! Do your knees have full extension?
Full knee extension is vital for walking, as it reduces stress on the joint when your body weight hits the ground. If extension is limited, the result is increased compression and rotational stress on joint surfaces. And as mentioned, rotation and compression are tough on cartilage. You’ve likely heard someone say, “My knee is bone on bone.” That’s from excessive cartilage loss.
Progressive loss of knee extension accelerates cartilage thinning, which—along with pain and limited function—determines when a joint needs to be replaced.
Other Contributing Factors
- Poor core and hip strength, leading to excessive thigh bone rotation into the knee
- Poor foot stability, creating rotation from below
- Excessive load on the quadriceps, increasing patellar stress
The theme here: Repetitive, excessive rotational stress on a joint not built to handle it. This leads to stiffness and degeneration over time, which forces the knee to cope with non-optimum conditions for good cartilage health.
The Good News
There’s a lot you can do to recover knee motion, improve flexibility, and build strength. At any stage, even after injury or accident, there is progress that can be made.
Unfortunately, many people go after the pain and inflammation in their joints with drugs instead of getting to the cause behind it. As long as Advil or Ibuprofen are the first line of defense, it’s going to be very difficult to observe the changes in function and range of motion and to interpret the signals the body is sending.
Painkillers may calm inflammation, but they don’t solve the root issue. Now, the question should be asked: did they contribute to the healing process? Did the cartilage in the joint heal fully, or is it now subtly weaker and wearing out faster?
Cartilage is a key part of joint health, and its longevity is a major factor in joint replacement. If you want to understand cartilage recovery, see our newsletter articles on “Wear Zones” and “Cartilage Health” under Health Tips on our website.
Final Thoughts
If you want to preserve your knees, keep your cartilage healthy, stay active later in life, and avoid a painful surgery followed by weeks of rehab, start paying attention now. Watch for small changes in your motion. Better yet, get evaluated by a movement expert at Full Potential PT. We’ll help you manage the friction and rotational stress that often lead to joint breakdown.
Don’t wait until you hear an orthopedist say, “When you can’t stand the pain anymore, schedule the knee replacement.” That’s a tough way to start retirement.
No matter your age, do the tests and see where you stand, or come in for a free consultation. We can help you identify the key stressors affecting your knees. And if you’re concerned about other joints—shoulder, hip, spine, or ankle—the same principles apply.
Give us a call or talk to your doctor about a referral, and your knees will thank you.

“I went from being non-weight bearing after my surgery to walking on the beach.“
“I went from being non-weight bearing after my surgery to walking on the beach. Thankful for the continued improvement each week! The things I enjoyed about Full Potential were:
- Tailored to my schedule, flexible
- Highly knowledgeable PTs
- Feedback on specifics like range of motion, building muscles to support the tendon, and long term plans and exercises.
Overall, physical therapy at Full Potential helped me improve 90%!” – Macall S.
Because every child entering foster care deserves dignity and comfort especially during a traumatic situation.
During the month of December, we will be collecting donations towards Hope Pkgs, a nonprofit that provides essential items for Michigan children placed into foster care. Hope Pkgs’ mission is not just to cover the necessities for children, but to give them a sense of comfort, dignity, and hope during a difficult and challenging time.
Here is your “heads up” to start collecting items now! We welcome donations of items like backpacks, underwear, socks, pajamas, toiletries, and more at the clinic throughout the month of December. For more information on Hope Pkgs or on what to donate, go to hopepkgs.org

Ask a PT
Welcome to our “Ask a PT” feature! This is your go-to spot in the newsletter to get real answers to everyday questions about the body, movement, and feeling your best. Whether you’re dealing with an injury, wondering how to stay active, or just curious about how physical therapy works, our team of physical therapists is ready to help. Each month we’ll share responses, tips, and answers based on questions from you, so if there’s something you’ve been wondering about, don’t be shy! Send it in – we’d love to hear from you!
Recent Q and A!
Q: I heard someone talking about the McKenzie Method for therapy. What is it and should I try it if I have pain?
A: The McKenzie Method (also called Mechanical Diagnosis and Therapy, or MDT) is a system used by physical therapists to assess and treat pain, especially back, neck, and joint pain. It focuses on finding specific movements that reduce your symptoms, then teaching you how to use those movements to manage pain on your own.
The McKenzie Method is great for people whose pain changes with movement or position — for example, if you have back pain and bending forward makes it worse, but arching back makes it better. One of the main goals is to help you become independent in managing your pain, so you don’t need to rely on constant hands-on treatment.
Should you try it?
If you’re having joint or back pain, you can use the McKenzie Method to help identify the source of your discomfort. If you’re looking for an active, long-term solution, it’s definitely worth exploring.
A great way to determine if it’s the right fit would be to set up a free consultation with one of our certified McKenzie physical therapists!
Q: I recently started running again and now I’m getting shin splints. How can I prevent them? How can I soothe them when they do come up?
A: Ah yes, shin splints — one of the most common (and annoying) issues runners face, especially when getting back into the swing of things! Great job getting back to running, by the way. The good news is that shin splints are very treatable and also preventable with a few smart changes.
“Shin splints” is a general term for pain along the inner edge of your shinbone (tibia). It’s caused by inflammation in the muscles, tendons, or even the bone tissue itself — usually from doing too much too soon. Kind of like we talked about in our main article, it’s one of the signals your body sends to say, “Let’s slow down a bit!”
To Prevent Shin Splints:
- Ease into running gradually — increase your mileage by less than 10% each week.
- Check your shoes — worn-out shoes or ones that don’t suit your foot type can throw off your mechanics.
- Run on softer surfaces — trails, treadmills, or tracks are easier on your legs than concrete.
- Strengthen your lower legs — exercises like toe raises, heel walks, and calf raises can build resilience.
- Warm up and cool down — don’t skip these! A brisk walk before and after your run helps immensely.
- Cross-train — mix in cycling, swimming, or strength training to reduce repetitive stress.
To Get Relief from Shin Splints:

- Rest and ease off running for a few days — swap in lower-impact activities like biking or walking.
- Ice your shins for 15–20 minutes at a time, especially after activity.
- Gently stretch your calves and lower legs to relieve tension.
- Massage or foam roll your calves and lower legs — but avoid directly massaging painful shin areas!
If your shin splints keep coming back or are getting worse, it may be due to an underlying issue like flat feet, tight calves, weak hips, or imbalanced stride mechanics. A physical therapist can help identify and correct these issues with a customized plan.
If you’d like to talk to a PT about your shin splints, reach out — and in the meantime, enjoy your running!
Don’t Let Your 2025 Insurance Benefits Go To Waste!
Take charge of your health today and make the most of your insurance benefits!
As the end of the year approaches (hard to believe 2026 is around the corner!), we want to remind you that now is a great time to take full advantage of your insurance benefits before they renew!
Most insurance plans renew in January. If you have already met or are close to meeting your deductible or out-of-pocket maximum, scheduling your care before your plan renews could help you save money and get the most of your benefits. Depending on your plan, it’s possible your care would be fully covered!
Please keep in mind that physical therapy typically involves a series of sessions over several weeks, so getting started now helps diminish the likelihood of your care extending into 2026.
Ready to make the most of your coverage? Call our office and we’ll be happy to provide a personalized insurance quote and help you schedule your first visit!

The Best Easy Pumpkin Pie Recipe
- 1 15-ounce can unseasoned pumpkin puree
- 2 teaspoons pumpkin pie spice
- 1/4 teaspoon salt
- 1 14-ounce can low-fat sweetened condensed milk
- 2 large eggs, lightly beaten
- 1 prepared pie crust, preferably whole-wheat, at room temperature
Position rack in lower third of oven. Preheat to 425°F.
Place pumpkin, pumpkin pie spice and salt in a medium bowl; whisk until combined. Add condensed milk and eggs; whisk until smooth. Pour into pie crust.
Bake for 15 minutes. Reduce the oven temperature to 350° and bake until the filling is set and a knife inserted in the center comes out clean, 35 to 40 minutes more. (Cover the crust edges with foil if they are browning too quickly.) Let cool completely, about 2 hours, before slicing.
Exercise of the Month
Hamstring Stretch
(Hamstrings, Low Back)
Start by lying on your back with both legs straight out. Loop a towel around your foot on the side you want to stretch. Keeping your leg as straight as possible, pull it up into the air using the ends of the towel. Hold when you feel a stretch in the back of your leg. Hold for 30 seconds. 3 Sets, 1 Rep. (Materials needed: towel)
Let’s Get You Better ASAP!
Don’t let pain dictate your life. Take the first step towards reclaiming your mobility and well-being with our expert support. Start your journey to a healthier you today.






